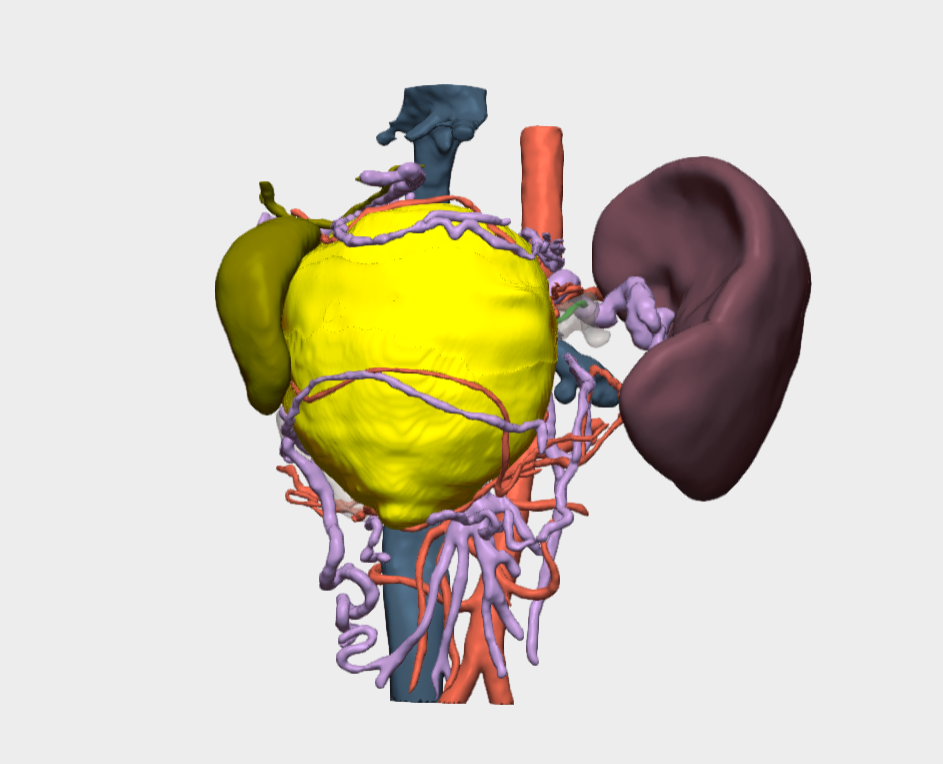
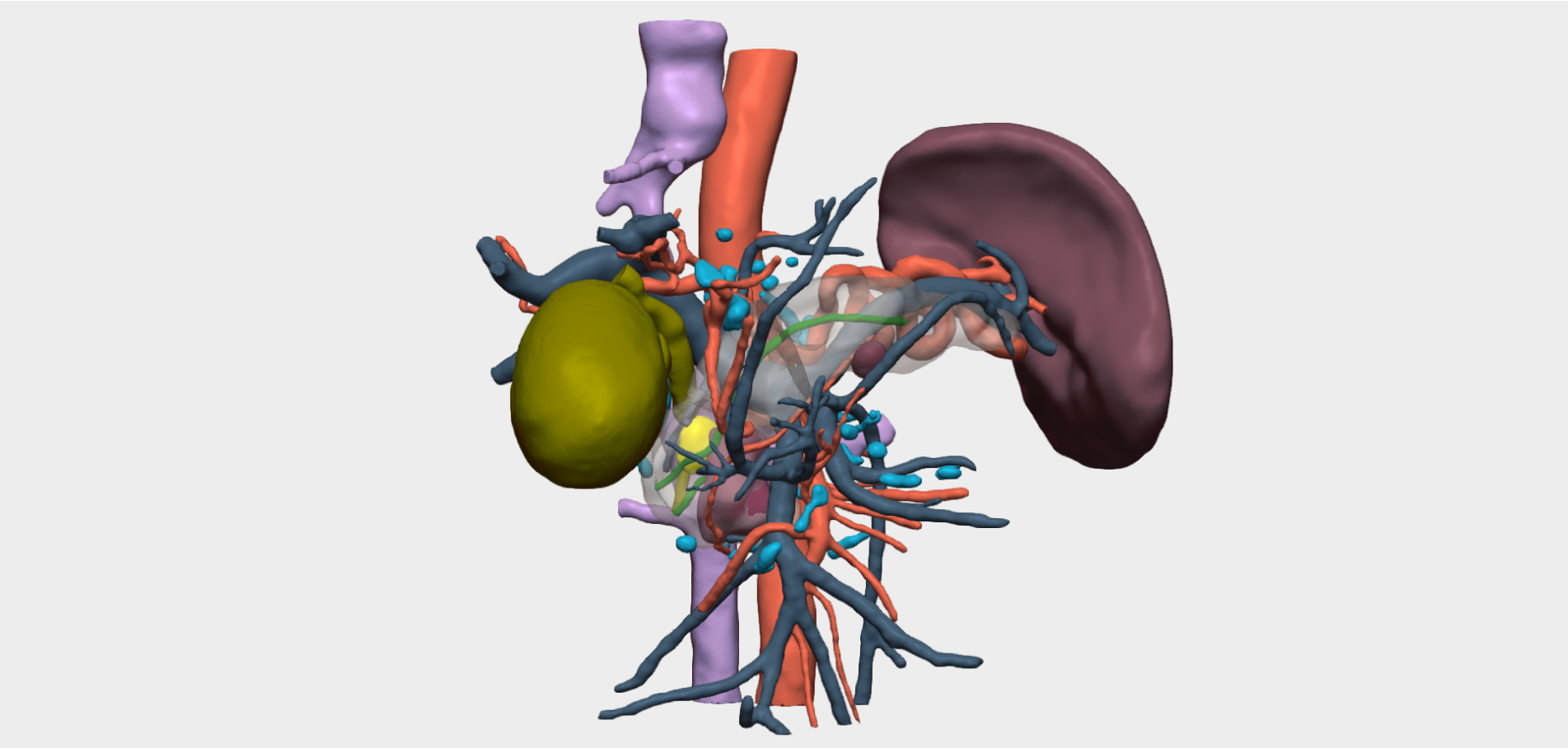
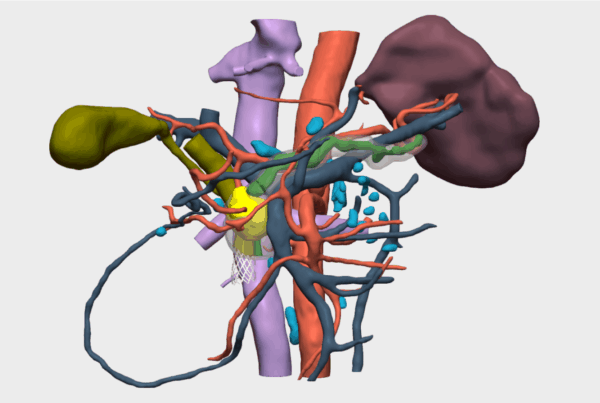
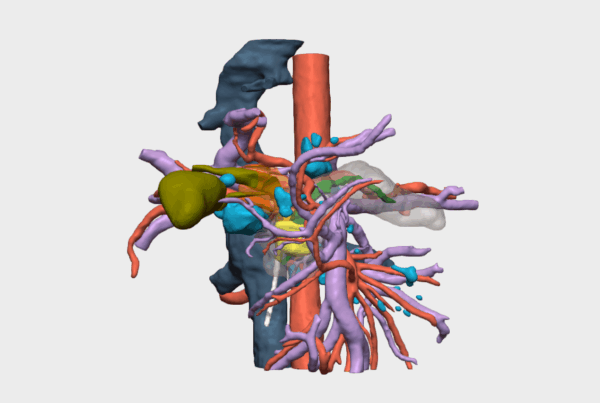
“The Cella 3D model enabled preoperative surgical simulation and, during the intraoperative phase, provided clear and precise guidance regarding the tumor’s relationship with key anatomical structures — in this case, the common bile duct, the hepatic artery, and the portal vein.”

Dr. Iván Bautista Hernández,, Pediatric Surgical Oncologist at the Teletón Children’s Oncology Hospital
Case Presentation
A 13-year-old female patient with a significant family history: paternal grandmother deceased at age 47 due to insulinoma, and cousins diagnosed with Addison’s disease currently under treatment. She first presented in March 2025, when an upper abdominal mass was detected and confirmed by ultrasound. During hospitalization, a contrast-enhanced CT scan revealed a pancreatic tumor. Endoscopic biopsy was performed, confirming the diagnosis of a solid pseudopapillary tumor of the pancreatic head (Frantz–Gruber tumor) with hepatic metastases.
The patient was referred to our institution for surgical management. Upon admission, she was in stable condition and asymptomatic.
3D Surgical Planning and Approach
The 3D model provided decisive value during surgery and contributed to:
- Preoperative simulation of the procedure and real-time intraoperative guidance.
- Clear and precise visualization of the tumor’s relationship with critical anatomical structures, specifically the common bile duct, hepatic artery, and portal vein.
- Identification of direct venous tributaries from the tumor to the portal vein and superior mesenteric vein, which were safely ligated and divided without intraoperative complications.
- Enhanced surgical planning through detailed visceral and vascular reconstructions, which were the key elements contributing to the success of the intervention.
The surgical strategy adopted was a pylorus-preserving pancreaticoduodenectomy (Whipple procedure).
Conclusions
The surgery was successfully completed without complications. Given the large size of the tumor, preoperative contrast-enhanced angio-CT imaging and the availability of the 3D model were essential for accurate surgical planning and for achieving a successful outcome.
The procedure was performed at the Hospital Infantil Teletón de Oncología, under the coordination of the Pediatric Surgical Oncology team, led by Dr. Iván Bautista Hernández, Pediatric Surgical Oncologist, together with Dr. Juan Manuel Alcántar Fierros, Pediatric Surgeon; Dr. Milen Montserrat Mendoza Ángeles, Medical Intern; Dr. Nayeli Bravo Santoyo, Anesthesiologist; and Dr. Jocelyn Zoraida Lugo Juárez, Pediatric Medical Oncologist.
¡Follow us on social media to stay up to date with our latest updates!